Varicose Veins
Say Goodbye to Varicose Veins: A Comprehensive Guide to Understanding, Treating and Preventing
by admin
26th September 2023
7 minutes read
Introduction
Varicose veins, an often unsightly and uncomfortable condition, have long been a source of frustration for many individuals worldwide. This common medical issue affects not only your physical appearance but also your quality of life, making even everyday activities a challenge. Thankfully, today’s advancements in medical science offer a myriad of options to effectively treat, manage and even say goodbye to varicose veins. In this blog post, we will delve deep into this topic, covering everything from symptoms to treatment options, and even preventative measures.
Understanding Varicose Veins
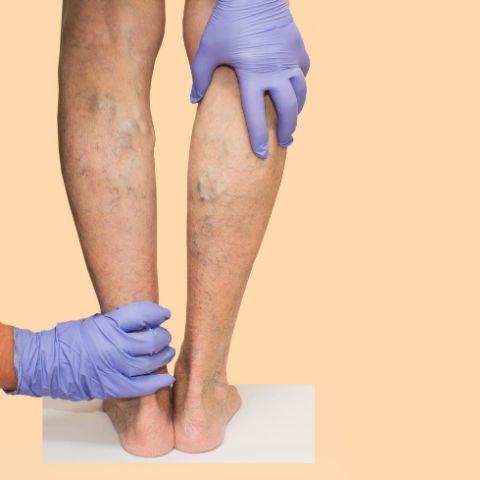
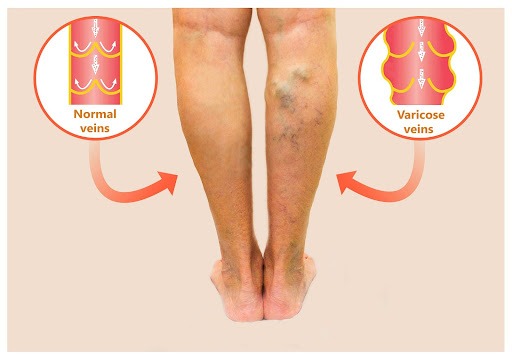
Varicose veins are large, swollen, and twisted veins that usually appear in the legs. These problematic veins are often blue or dark purple and are sometimes lumpy, bulging or twisted in appearance. This happens when the valves within the veins do not work effectively, causing blood to collect and pressure to build, leading to enlarged, visible veins on the legs.
Symptoms of Varicose Veins
Varicose veins are often identifiable by their appearance: they’re enlarged, swollen, and over time can become twisted and turn a blue or dark purple colour. However, the condition can also present a range of other symptoms. Here are the common signs and symptoms of varicose veins:
- Aching Legs: Your legs may feel heavy and achy, especially after standing for long periods. This is due to poor circulation and the increased pressure in the veins.
- Swollen Ankles and Feet: As varicose veins worsen, they can lead to fluid buildup resulting in swollen ankles and feet.
- Itching: Some people may experience itching around one or more of their veins. In some cases, this can also indicate a skin infection or skin ulcers due to the varicose veins.
- Cramping or Throbbing: Your legs may cramp or throb at night. The cramping can sometimes be severe enough to wake you up from sleep.
- Changes in Skin Colour: Over time, you may notice changes in the colour of the skin on your legs and around your ankles. The skin can become darker, harder, or thicker due to the increased pressure in the veins.
- Visible Veins: This is often the most noticeable symptom. The veins in your legs become large, swollen and twisted, and are visible under the skin.
- Restless Legs Syndrome: Some people with varicose veins also experience restless legs syndrome, a condition characterised by an uncomfortable sensation that makes you want to move your legs, particularly at night or when sitting for long periods.
If you are experiencing these symptoms, it’s important to consult a healthcare provider. While varicose veins are usually not a serious condition, they can lead to complications if left untreated. Plus, treatments can help reduce symptoms and improve the appearance of your legs.
Are Varicose Veins Dangerous?
Varicose veins are usually not dangerous, but they can cause discomfort and pain, and sometimes lead to complications if left untreated. While most people seek treatment for cosmetic reasons or due to discomfort, some people might experience more serious issues related to varicose veins.
Here are a few potential complications that can arise from untreated varicose veins:
- Venous Insufficiency: This condition occurs when your leg veins do not allow blood to flow back to your heart. Chronic venous insufficiency can lead to changes in the skin, skin ulcers, and infection.
- Blood Clots: Deep vein thrombosis (DVT) can occur when varicose veins lead to blood clots in veins deeper within the legs. This condition can be life-threatening if a blood clot breaks loose and travels to the lungs, causing a pulmonary embolism.
- Bleeding: Varicose veins near the surface of your skin may occasionally bleed if you scratch or cut your skin. The bleeding may be difficult to stop. Elevated pressure within the vein can also cause spontaneous bleeding.
- Superficial Thrombophlebitis: This condition, characterised by a blood clot in a vein just beneath the surface of the skin, can lead to swelling, redness, and tenderness over the affected vein.
- Skin Ulcers: These painful ulcers usually form on the skin near varicose veins, particularly near the ankles. They require immediate medical attention.
These complications are relatively rare but can be severe. If you are experiencing any symptoms of varicose veins, it is important to consult a healthcare provider to evaluate your symptoms and discuss treatment options. Prevention and timely treatment are key to managing this condition.
Varicose Veins Treatment
Thankfully, there are numerous varicose vein treatments available, which vary in nature and cost. Here are some of the options:
Varicose Vein Surgery
In severe cases, varicose veins surgery may be recommended. This procedure typically involves the removal of the problematic veins (varicose vein removal), which forces the blood to flow through healthier veins. While this method is effective, it can be invasive and may require a longer recovery time.
Laser Treatment for Varicose Veins
Laser treatment is a less invasive alternative for varicose veins. In this procedure, a thin fiber is inserted into the vein, which emits laser energy that heats and closes off the vein. Varicose veins laser treatment cost can vary widely depending on the severity of your condition and the healthcare provider.
Varicose Veins Medicine
In some cases, your doctor may prescribe medicines to help manage the symptoms of varicose veins. These could include pain relievers, diuretics to reduce swelling, or anticoagulants to prevent blood clots. It’s important to note that medication does not cure varicose veins but can help manage the symptoms and prevent complications.
Preventing Varicose Veins
While treatments are important, prevention is always the best approach. Regular exercise, maintaining a healthy weight, avoiding long periods of sitting or standing, and wearing compression stockings can help prevent varicose veins or keep them from getting worse.
Conclusion
Living with varicose veins can be both physically uncomfortable and emotionally draining. However, it’s essential to remember that you’re not alone and that help is available. With the wide variety of treatment options now available, you can effectively manage, treat and even say goodbye to varicose veins for good. Whether it’s a less invasive laser treatment or a more comprehensive varicose veins medical procedure, the first step is always to consult with a specialist. Do your research, find a veins doctor near you, and embark on your journey towards a varicose-free life.
How can Medfin help?
Medfin Health Care offers comprehensive support for Varicose Veins. Experience hassle-free care as we connect you with top specialists, ensuring effective treatment. Choose Medfin to prioritize your vascular health and enjoy a smoother journey towards healthier veins.!
FAQs
1. Is there any way to prevent varicose veins from developing?
While some factors contributing to varicose veins, such as genetics, cannot be changed, you can take preventive measures. Regular exercise, maintaining a healthy weight, avoiding excessive heat exposure, and elevating your legs can help reduce the risk.
2. Can pregnancy cause varicose veins?
Yes, pregnancy is a common risk factor for developing varicose veins. The increased blood volume and pressure on the veins from the growing uterus can contribute to their formation.
3. How long is the recovery period after varicose vein treatment?
The recovery period varies depending on the treatment method used. Minimally invasive procedures usually have shorter recovery times compared to traditional surgery. In most cases, patients can return to normal activities within a few days to a week. However, it’s essential to follow the doctor’s post-treatment instructions for the best outcome.
4. Can lifestyle changes help reduce varicose veins?
Yes, certain lifestyle changes can help alleviate symptoms and reduce the risk of developing varicose veins. Regular exercise, maintaining a healthy weight, avoiding prolonged sitting or standing, and elevating your legs can be beneficial.
5. At what age do varicose veins typically appear?
Varicose veins can develop at any age, but they are more common in older individuals, usually appearing between the ages of 30 and 70.
CATEGORIES
- ACL Reconstruction
- Anal Fissures
- Anal Fistula
- Appendicitis
- ASK A DOCTOR
- Benign Prostatic Hyperplasia
- Breast Lump Excision
- Cataract
- Circumcision
- Conditions & Diseases
- Cosmetology
- Covid-19
- Cure
- Endocrinology
- ENGLISH VIDEOS
- Eye Care
- Gallstones
- General Surgeries
- Government Schemes
- Gynaecology
- Gynecomastia
- Health
- Health Insurance
- Hernia
- Hindi
- Hip Arthoscopy
- Hip Replacement
- Hip Replacement Surgery
- Hydrocele
- Kannada
- Kidney Stones
- Knee Arthroscopic
- Laparoscopic
- LASER
- Latest Treatments
- Lifestyle
- Liposuction
- Medfin Stories
- Medicine
- Nephrology
- Ophthalmology
- Orthopaedic
- Paraphimosis
- Patient Testimonials
- PCL Reconstruction
- Phimosis
- Piles (Hemorrhoids)
- Pilonidal Sinus
- Proctology
- Prostate Artery Embolization
- Rhinoplasty
- Second Opinion
- Total Knee Replacement
- Urology
- Uterine Artery Embolization
- Uterine Fibroids
- Varicocele
- Varicose Veins
- Vascular
- VIDEOS